Scoliosis & Spinal Deformities
Scoliosis and spinal deformities refer to abnormal curvature or alignment of the spine that can affect posture, balance, and spinal mechanics. Symptoms range from cosmetic changes and back pain to nerve irritation and functional limitations.
Common Symptoms
- Uneven shoulders, hips, or waistline
- Visible spinal curve or rib prominence
- Mid-back or low back pain and fatigue
- In some cases: leg pain, numbness, or weakness
Common Causes
- Idiopathic scoliosis (no clear cause, often develops in adolescence)
- Degenerative changes (adult scoliosis)
- Congenital or neuromuscular conditions
- Prior spine surgery or structural imbalance
Insurance check, handled.
We’ll verify benefits and walk you through expected coverage before treatment. No surprises.
- Benefit verification before major steps
- Clear scheduling + documentation support
- Help coordinating imaging when needed
What Are Scoliosis and Spinal Deformities?
Scoliosis is an abnormal curvature of the spine, most commonly a side-to-side (coronal) curve that can also involve rotation of the vertebrae. “Spinal deformity” is a broader term that includes scoliosis as well as other alignment issues, such as abnormal forward bend (kyphosis) or excessive inward curve (lordosis).
In adults, scoliosis often develops from degeneration of discs and joints over time (degenerative scoliosis) and may be associated with spinal stenosis or nerve irritation. In adolescents, idiopathic scoliosis is the most common type and may be discovered during growth spurts.
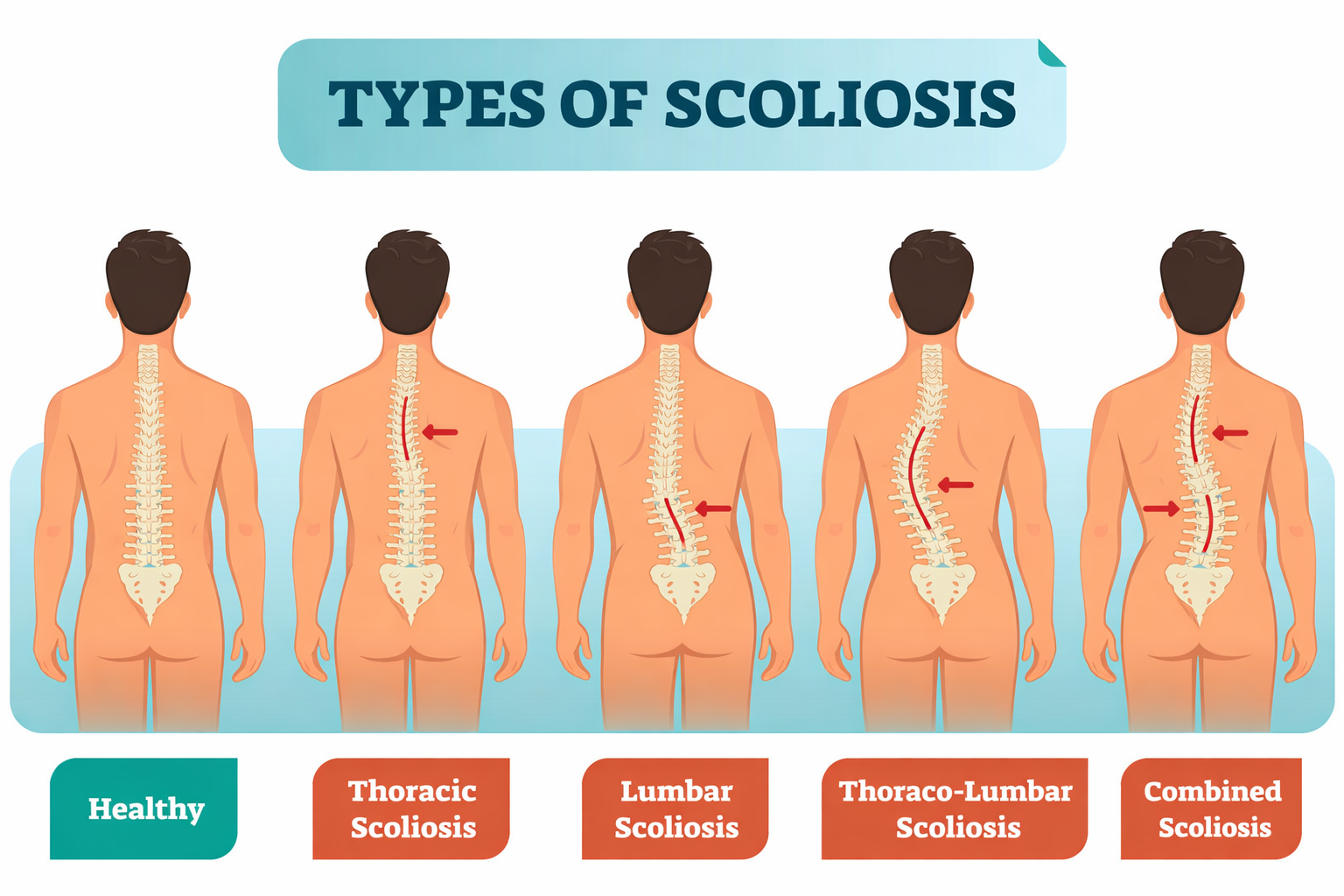
Illustration showing scoliosis with abnormal spinal curvature and alignment.
Why It Matters
Spinal deformities can change how weight and forces move through the spine. Over time, this can contribute to pain, muscle fatigue, joint degeneration, and in some cases nerve compression that causes radiating pain, numbness, or weakness.
When It Needs Prompt Evaluation
Progressive weakness, worsening balance, significant radiating leg or arm symptoms, or new bowel/bladder changes should be evaluated promptly. These can indicate nerve or spinal cord involvement.
Symptom Check
This quick check helps sort common scoliosis/deformity symptom patterns and flags symptoms that should be evaluated sooner. It’s not a diagnosis.
Scoliosis / Deformity Triage
5 questions • helps route common patterns
1) Any urgent symptoms right now?
2) What’s the main reason you’re looking this up?
3) Age group?
4) Are symptoms getting worse over time?
5) Are there nerve symptoms (radiating leg/arm pain, numbness, tingling)?
Diagnosis
Diagnosis starts with a physical exam and a review of symptoms and function. Imaging helps measure the degree of curvature, evaluate alignment, and identify any nerve compression or degeneration that may be contributing to pain.
Clinical Exam
- Posture, shoulder/hip alignment, and gait assessment
- Range of motion and pain pattern review
- Strength, sensation, and reflex testing
Imaging
- Standing spine X-rays (curve measurement and alignment)
- MRI (if nerve symptoms are present)
- CT (bone detail, selected cases)
Additional Tests
- Bone density testing (selected adult patients)
- EMG/NCS (if needed for nerve function)
Treatment
Treatment depends on the type of deformity, curve severity, symptoms, and how much it impacts daily function. Many patients respond well to non-surgical care. Surgery may be considered for progressive deformity, significant pain, or neurological symptoms due to nerve compression.
Non-Surgical Options
- Physical therapy (core strength, posture, mobility)
- Targeted exercise programs for spinal stability
- Activity modification and ergonomic changes
- Anti-inflammatory medications (NSAIDs) when appropriate
- Spinal injections for pain or nerve irritation (selected cases)
- Bracing (primarily for adolescents; selected adult cases)
Surgical Options
- Decompression for nerve compression (selected cases)
- Spinal fusion to correct and stabilize the curve
- Realignment procedures for significant deformity
- Minimally invasive approaches when appropriate
Recovery
Recovery varies depending on curve severity and the treatment plan. Non-surgical care focuses on improving strength and endurance. Surgical recovery depends on the type of correction and stabilization performed and typically includes a structured rehab plan.
Conservative Care
- Improvement builds with consistent therapy
- Strength and endurance can reduce pain over time
- Long-term maintenance plan is important
After Injections
- Relief may start within days to ~2 weeks
- Best paired with rehab and posture changes
- Repeat only when clinically appropriate
After Surgery
- Early mobility is encouraged in most cases
- Restrictions depend on procedure type and levels treated
- PT is commonly recommended as part of recovery
Prevention
Not all deformities are preventable, but strong spine mechanics and early evaluation can reduce progression risk and improve long-term outcomes—especially for adolescents during growth and adults with degenerative changes.
Daily Habits
- Maintain neutral posture and ergonomic setup
- Take breaks from prolonged sitting
- Use proper lifting mechanics
- Monitor symptoms and function over time
Strength & Mobility
- Core and hip strengthening
- Upper back and scapular strengthening
- Mobility work for stiffness and imbalance
- Low-impact conditioning consistency
FAQ
Is scoliosis always painful?
No. Many people have scoliosis without pain. When pain occurs, it may be related to muscle fatigue, arthritis, or nerve compression associated with degenerative changes.
Can scoliosis get worse over time?
It can. Adolescent curves can progress during growth, and adult degenerative scoliosis may worsen gradually over time. Monitoring with imaging and symptom tracking helps guide treatment decisions.
When is surgery considered?
Surgery may be considered for progressive deformity, significant pain that doesn’t respond to conservative care, or neurological symptoms caused by nerve compression. The goal is to stabilize the spine, protect nerves, and improve alignment and function.
Can adults develop scoliosis later in life?
Yes. Degenerative scoliosis can develop over time from disc and joint wear, often alongside stenosis. Symptoms can include back fatigue, asymmetry, and sometimes leg symptoms from nerve compression.
Schedule a consultation
We’ll review symptoms, alignment, and imaging and walk through options—non-surgical or surgical—based on your goals.
If you have worsening weakness, falls, or bowel/bladder changes, seek urgent evaluation.
What to bring
- Prior X-rays/MRI/CT reports (if available)
- Medication list
- Timeline of symptoms and what triggers them
- Any leg/arm numbness, tingling, or weakness details
