Spinal Cord Compression
Spinal cord compression happens when pressure on the spinal cord interferes with nerve signals. It can cause pain, numbness, weakness, balance problems, or coordination changes. Because the spinal cord controls strength and sensation below the compressed area, progressive symptoms should be evaluated promptly.
Common Symptoms
- Weakness in arms or legs
- Balance or coordination problems
- Numbness, tingling, or heaviness
- Hand clumsiness (buttoning, writing, grip)
Common Causes
- Disc herniation or disc bulge
- Spinal stenosis (narrowing around the cord)
- Bone spurs / arthritis (spondylosis)
- Trauma, tumor, infection (less common)
Insurance check, handled.
We can verify benefits, coordinate imaging, and lay out the next step once results are in.
- Benefit verification before procedures
- Help coordinating MRI/CT orders
- Clear plan after imaging
What Is Spinal Cord Compression?
The spinal cord is the “main cable” that carries signals between your brain and the body. Spinal cord compression occurs when something narrows the space around the cord or presses on it—reducing normal nerve signal flow.
Symptoms can start subtly (hand clumsiness, balance changes, heaviness in the legs) and may progress over time. Because the spinal cord does not tolerate pressure well, worsening neurologic symptoms should be evaluated promptly.
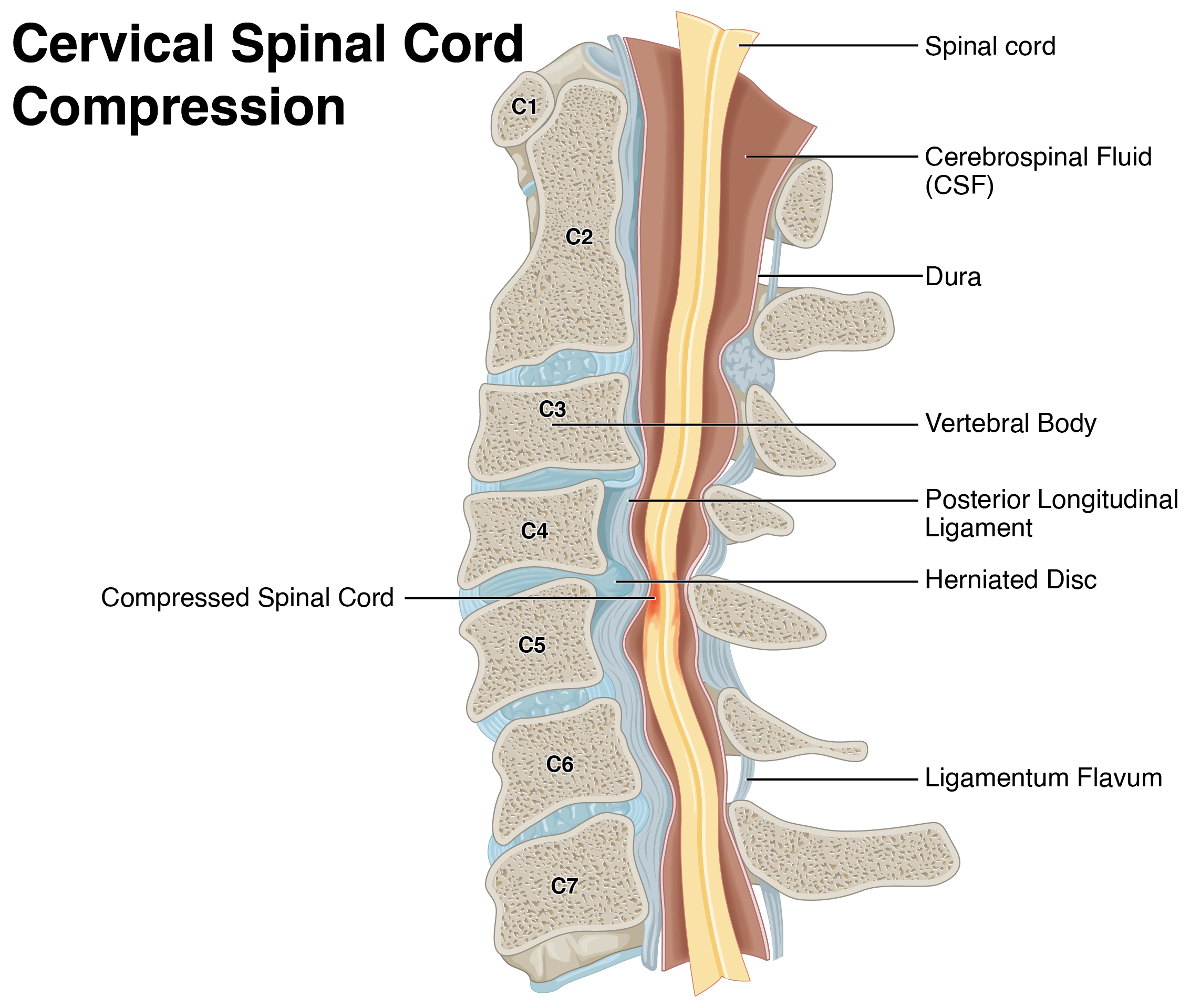
Illustration showing pressure on the spinal cord that can affect strength, sensation, and coordination.
Why It Can Be Serious
Ongoing compression can lead to progressive weakness, coordination problems, and difficulty walking. Treatment is often focused on protecting function and preventing worsening.
What “Myelopathy” Means
Myelopathy is a term for spinal cord dysfunction. It can show up as balance problems, hand clumsiness, heaviness in the legs, or changes in reflexes.
Emergency Check
Quick check to help you decide urgency. This is not a diagnosis.
Spinal Cord Compression Triage
5 questions • flags urgent vs routine evaluation
1) Any new or worsening weakness?
2) Any trouble walking or major balance change?
3) Any bowel/bladder changes or saddle numbness?
4) Symptoms getting worse over days/weeks?
5) Any fever, cancer history, or recent major injury?
Diagnosis
Diagnosis includes a focused neurological exam and imaging to confirm whether the spinal cord is compressed, where it’s happening, and what’s causing it. The key question is whether symptoms and imaging suggest spinal cord dysfunction (myelopathy).
Clinical Exam
- Strength, sensation, reflexes
- Balance, gait, coordination testing
- Hand dexterity + fine motor assessment
Imaging
- MRI (best for spinal cord + soft tissue)
- X-rays (alignment/instability)
- CT (bone spurs/fracture detail, selected cases)
Additional Workup
- Review of prior imaging and symptom timeline
- Lab testing (selected cases)
- Referral/coordination if tumor or infection is suspected
Treatment
Treatment depends on the cause and how the spinal cord is affected. Mild, stable symptoms may start with conservative care and close monitoring. Progressive neurologic changes or significant cord compression may require surgical decompression.
Non-Surgical Options
- Activity modification + symptom management
- Physical therapy focused on safe mobility/strength
- Anti-inflammatory meds (NSAIDs) when appropriate
- Short-term oral steroids (selected cases)
- Close monitoring for progression
Surgical Options
- Decompression to relieve spinal cord pressure
- Procedure depends on cause (disc, bone spur, stenosis)
- Stabilization/fusion when indicated
- Minimally invasive approaches in selected cases
Recovery
Recovery depends on how long the cord has been compressed, severity of symptoms, and the treatment approach. Many patients see improvement in function over time, but in some cases the main goal is preventing worsening.
Conservative Care
- Best for mild, stable symptoms
- Focus on mobility, strength, fall-risk reduction
- Follow-up is important
After Surgery
- Early mobility is encouraged in most cases
- Restrictions depend on the procedure performed
- PT may be recommended
Expected Progress
- Improvements may continue over months
- Earlier treatment often leads to better outcomes
- Main goal may be preventing worsening
Prevention
Not all causes are preventable, but reducing flare-ups and protecting function starts with early evaluation of neurologic symptoms, staying active safely, and addressing posture/ergonomics.
Daily Habits
- Maintain good posture and ergonomic setup
- Take breaks from prolonged sitting
- Stay active with low-impact conditioning
- Don’t “push through” progressive neurologic symptoms
Strength & Mobility
- Core and upper back strengthening
- Balance training when appropriate
- Mobility work to reduce stiffness
- Gradual progression with exercise
FAQ
Is spinal cord compression an emergency?
It can be. New or progressive weakness, trouble walking, loss of coordination, or bowel/bladder changes should be treated as urgent.
What’s the best test to confirm spinal cord compression?
MRI is typically the best test because it shows the spinal cord and soft tissues clearly.
Does spinal cord compression always require surgery?
Not always. Mild, stable symptoms may be treated non-surgically with close monitoring. Surgery is considered when symptoms progress or imaging shows significant cord compression that matches neurologic findings.
Schedule a consultation
We’ll review symptoms and imaging and coordinate the safest next step.
If you have worsening weakness, trouble walking, or bowel/bladder changes, seek urgent evaluation.
What to bring
- MRI/CT/X-ray reports and image discs/links
- Medication list
- Timeline of symptoms
- Prior treatments tried (PT, injections, meds)
