Facet Joint Syndrome
Facet joints are the small stabilizing joints at the back of the spine. When they become inflamed or arthritic, they can cause neck or back pain and stiffness—often worse with arching backward, twisting, or prolonged standing.
Common Symptoms
- Localized neck or low back pain (often one-sided)
- Stiffness, especially after rest
- Pain worse with extension (arching backward)
- Pain with twisting, prolonged standing, or walking
What It Usually Is Not
- True shooting pain past the elbow/knee (more typical of nerve irritation)
- Progressive weakness
- New bowel/bladder changes
- Rapidly worsening numbness
Insurance check, handled.
We can verify benefits, coordinate imaging, and explain next steps if injections or other procedures are recommended.
- Benefit verification before procedures
- Help coordinating X-ray/MRI orders
- Clear plan after imaging
What Is Facet Joint Syndrome?
Facet joints connect one vertebra to the next and help guide spinal motion. Over time, these joints can become irritated from arthritis, increased mechanical load, or inflammation after a strain.
Facet pain is commonly worse with extension (arching backward), rotation, and prolonged standing. It may feel deep, achy, and stiff, and can refer into nearby areas (buttock/hip or shoulder blade) without true nerve compression.
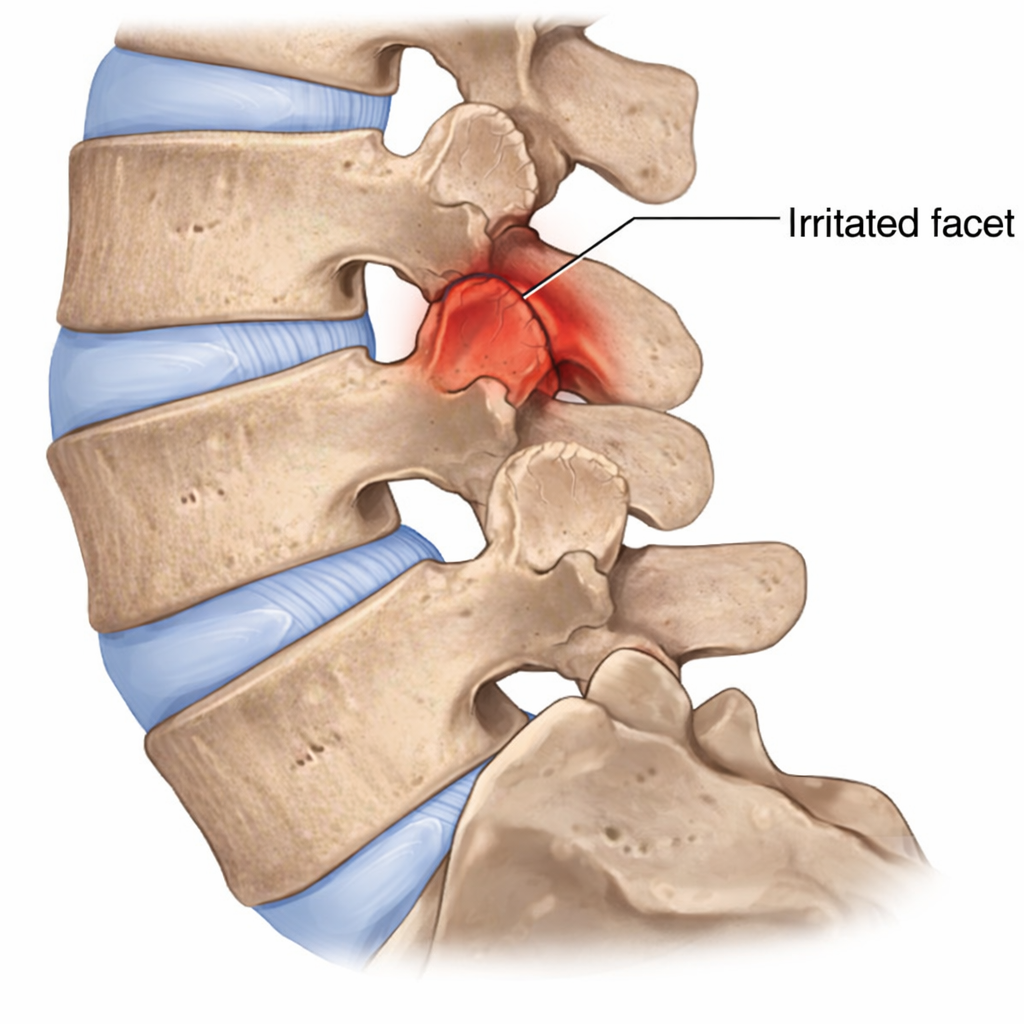
Illustration showing facet joints and common pain sources.
Why It Happens
As discs lose height (degeneration), facet joints can take on more load. The joints can become inflamed and painful, similar to arthritis in other parts of the body.
When to Think “Nerve” Instead
If pain shoots down the arm/leg with numbness/tingling or weakness, that may indicate nerve irritation and needs evaluation.
Quick Check
Quick screen for urgency. Not a diagnosis.
Facet Pain Triage
5 questions • flags urgent vs routine evaluation
1) Any bowel/bladder changes or saddle numbness?
2) Any weakness or rapidly worsening numbness/tingling?
3) Does pain shoot past the elbow/knee?
4) Is pain worse with arching backward or twisting?
5) Is pain improving with conservative care (rest/NSAIDs/PT)?
Diagnosis
Diagnosis combines your symptom pattern, exam findings, and imaging. Because several structures can mimic each other, diagnostic injections may be used to confirm the facet joints as the primary pain source.
Clinical Exam
- Extension/rotation provocation
- Posture and movement mechanics
- Neurologic exam if radiating symptoms exist
Imaging
- X-rays (arthritis and alignment)
- MRI (rules out disc/nerve compression)
- CT (bone detail in selected cases)
Confirming the Pain Source
- Medial branch blocks (diagnostic)
- Facet joint injections (selected cases)
- Response to blocks guides next steps
Treatment
Most facet pain improves with conservative care. If symptoms persist, targeted procedures can reduce inflammation and help you progress through rehab.
Non-Surgical Options
- Physical therapy (core stability, mobility, posture)
- NSAIDs when appropriate
- Heat/ice and home exercise program
- Ergonomic and activity modifications
Procedures (Selected Cases)
- Facet injections for inflammation
- Medial branch blocks (to confirm facet source)
- Radiofrequency ablation (RFA) if blocks confirm facets
Recovery
Recovery depends on how consistent the rehab plan is. Procedures can reduce pain, but strength and mechanics are what keep it controlled.
Conservative Care
- Improvement usually builds over weeks
- Expect flare-ups early—plan for them
- Maintenance routine prevents recurrence
After Injections
- Relief may start within days to ~2 weeks
- Best paired with strengthening
- Repeat only when clinically appropriate
After RFA
- Often takes 1–3 weeks to fully kick in
- Relief can last months in selected cases
- Continue rehab to maintain results
Prevention
Facet joints dislike repeated extension/rotation under load. Good mechanics and strength reduce repeat overload.
Daily Habits
- Break up long standing/sitting
- Keep spine neutral during lifting
- Adjust workstation ergonomics
- Progress activity gradually
Strength & Mobility
- Core + hip strengthening
- Thoracic mobility (for neck/back mechanics)
- Glute strength to reduce lumbar load
- Low-impact conditioning
FAQ
How is facet pain different from a pinched nerve?
Facet pain is usually localized and worse with arching backward or twisting. A pinched nerve more often causes shooting pain, numbness/tingling, or weakness down the arm or leg.
What is RFA?
Radiofrequency ablation targets the small nerves that transmit pain signals from the facet joints. It’s typically considered after diagnostic blocks confirm the facet joints are the main pain source.
Do injections cure facet arthritis?
They can reduce inflammation and pain, but long-term control usually depends on mechanics and strengthening to reduce repeat overload.
Schedule a consultation
We’ll confirm the pain source and build the simplest plan that gets you better.
If you have weakness, bowel/bladder changes, or worsening numbness/tingling, seek urgent evaluation.
What to bring
- Any prior imaging reports (X-ray/MRI/CT)
- Medication list
- Timeline of symptoms and triggers
- Prior PT/injection history
