Spinal Arthritis (Spondylosis)
Spondylosis is arthritis and wear-and-tear of the spine. Over time, discs and joints can degenerate and form bone spurs, causing stiffness and pain. If narrowing develops, it can irritate nerves—or in the neck, compress the spinal cord.
Common Symptoms
- Neck or back pain with stiffness
- Reduced range of motion
- Muscle tightness/spasm
- Sometimes: radiating pain, numbness, tingling, weakness
Common Drivers
- Disc degeneration + facet arthritis
- Bone spurs (osteophytes)
- Thickened ligaments and joint changes
- Prior injury or repetitive mechanical stress
Insurance check, handled.
We can verify benefits, help coordinate imaging, and explain next steps once results are in.
- Benefit verification before procedures
- Help coordinating MRI orders
- Clear plan after imaging
What Is Spinal Arthritis?
Spinal arthritis (spondylosis) describes degenerative changes involving discs, facet joints, and bone spurs. Many people have these changes on imaging without severe symptoms.
Symptoms can come from inflammation (stiffness and local pain), nerve irritation (radiating pain/numbness), or narrowing (stenosis). In the cervical spine, cord compression can present as balance issues or hand clumsiness.
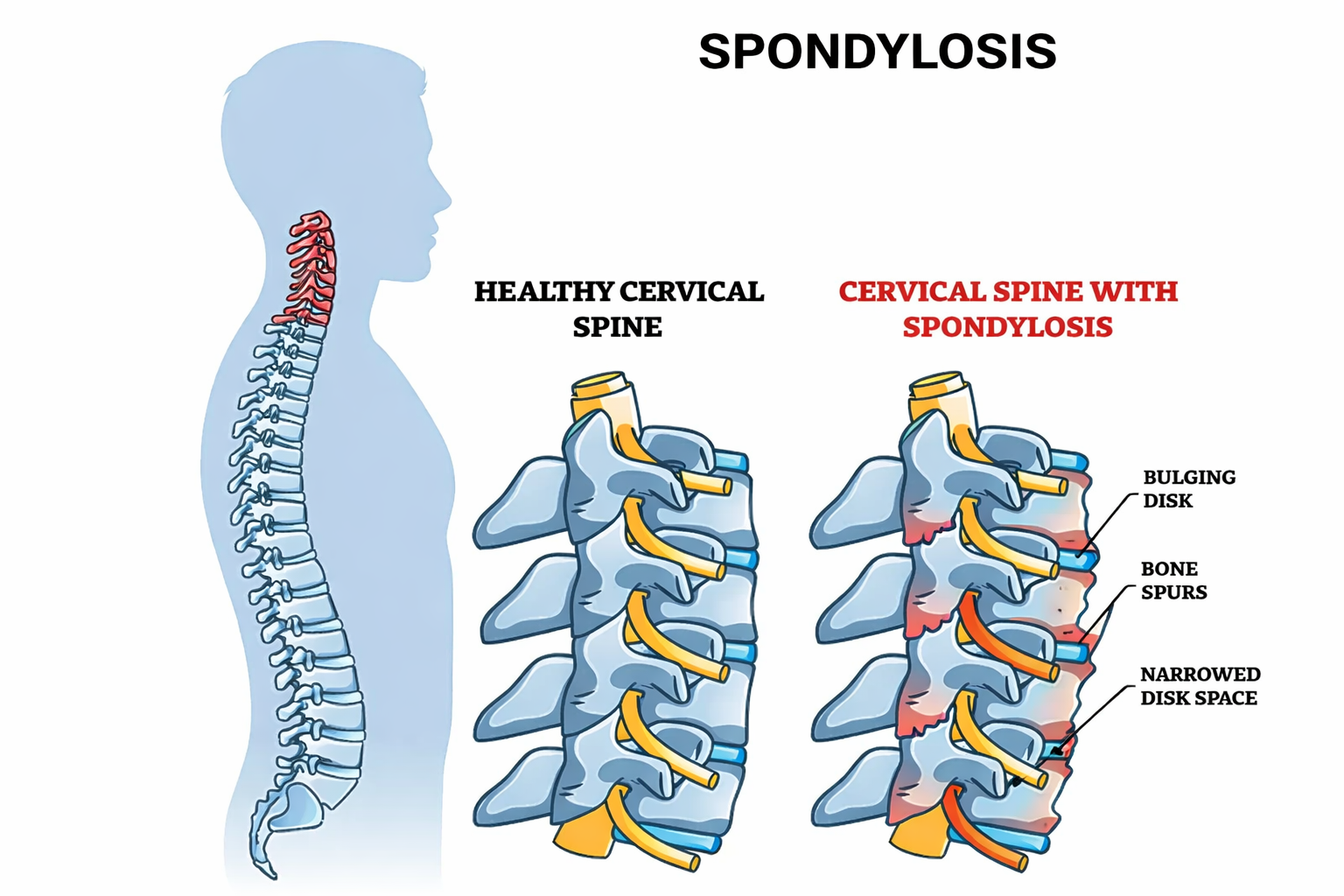
Illustration showing arthritis changes and bone spurs that can narrow space for nerves.
Why Symptoms Happen
Arthritis can inflame joints and stiffen the spine. Bone spurs and ligament thickening can narrow the canal or foramina, irritating nerves and causing radiating pain, numbness, tingling, or weakness.
When It Needs Prompt Evaluation
Worsening weakness, trouble walking, balance changes, or hand clumsiness can indicate spinal cord involvement and should be evaluated promptly.
Quick Check
Quick screen for urgency. Not a diagnosis.
Spondylosis Symptom Check
5 questions • flags urgent vs routine evaluation
1) Any bowel/bladder changes or saddle numbness?
2) Any worsening weakness in arms or legs?
3) Balance issues, frequent falls, or walking changes?
4) Hand clumsiness or dropping objects?
5) Are symptoms persistent despite conservative care?
Diagnosis
Diagnosis combines exam findings with imaging to confirm arthritis changes and determine whether nerves or the spinal cord are involved.
Clinical Exam
- Range of motion and pain triggers
- Strength, sensation, reflex testing
- Gait/balance evaluation when indicated
Imaging
- X-rays (arthritis, spurs, alignment)
- MRI (nerves/spinal cord, stenosis)
- CT (bone detail, selected cases)
Helpful Add-ons
- Diagnostic injections (selected cases)
- EMG/NCS if symptoms are unclear
- Review of prior imaging if available
Treatment
Treatment focuses on reducing inflammation, improving mechanics, and protecting nerves if narrowing is present. Most patients improve without surgery.
Non-Surgical Options
- Physical therapy (mobility, strength, posture)
- NSAIDs when appropriate
- Heat/ice and home exercise program
- Injections for inflammation or nerve irritation (selected cases)
- Activity modification + ergonomic improvements
Surgical Options (Selected Cases)
- Decompression if nerves/spinal cord are compressed
- Stabilization/fusion if instability is present
- Approach depends on level(s) and severity
Recovery
Arthritis is long-term, but symptoms are often controllable with a consistent plan.
Conservative Care
- Expect gradual improvement over weeks
- Consistency reduces flare-ups
- Maintenance plan is key
After Injections
- Relief may start within days to ~2 weeks
- Best paired with rehab
- Repeat only when clinically appropriate
After Surgery
- Recovery depends on procedure type
- PT is often part of recovery
- Improvement can continue for months
Prevention
You can’t stop aging, but you can reduce flare-ups and protect function.
Daily Habits
- Ergonomics and posture
- Break up prolonged sitting/standing
- Safe lifting mechanics
- Gradual activity progression
Strength & Mobility
- Core + hip strengthening
- Mobility work for stiffness
- Low-impact conditioning
- Balance work when needed
FAQ
What does “spondylosis” mean on imaging?
It usually refers to degenerative arthritis changes—disc wear, facet joint arthritis, and sometimes bone spurs.
Can spondylosis cause nerve symptoms?
Yes. Narrowing can irritate nerves and cause radiating pain, numbness, tingling, or weakness.
When is surgery considered?
Surgery is considered when there is significant nerve/spinal cord compression, progressive neurologic deficits, or instability.
Schedule a consultation
We’ll review symptoms and imaging and coordinate the safest next step.
If you have balance changes, weakness, or bowel/bladder symptoms, seek urgent evaluation.
What to bring
- X-ray/MRI reports and images (if available)
- Medication list
- Timeline of symptoms and function changes
- Prior PT/injection history
