Spinal Tumors
Spinal tumors are abnormal growths that develop in or near the spine. They can involve the vertebrae, spinal cord, or surrounding tissues and may cause back or neck pain, nerve symptoms, weakness, or balance changes depending on location.
Common Symptoms
- Persistent back or neck pain (often worse at night)
- Radiating arm or leg pain, numbness, or tingling
- Weakness or coordination changes
- Unexplained weight loss or systemic symptoms (in some cases)
Common Types / Causes
- Benign tumors (non-cancerous growths)
- Malignant tumors (cancerous growths)
- Metastatic tumors (spread from another cancer)
- Primary spine tumors (originate in the spine)
Insurance check, handled.
We’ll verify benefits and walk you through expected coverage before major steps. No surprises.
- Benefit verification before procedures
- Help coordinating imaging orders
- Clear next steps after results
What Are Spinal Tumors?
Spinal tumors are abnormal growths that form in or around the spine. They may develop in the vertebrae (bones), within the spinal canal, or in tissues near the spine. Tumors can be benign (non-cancerous) or malignant (cancerous), and some tumors represent metastasis, meaning cancer spread from another part of the body.
Symptoms depend on tumor location and whether it causes instability or compresses nerves or the spinal cord. Because spinal cord and nerve compression can worsen over time, new or progressive neurological symptoms require prompt evaluation.
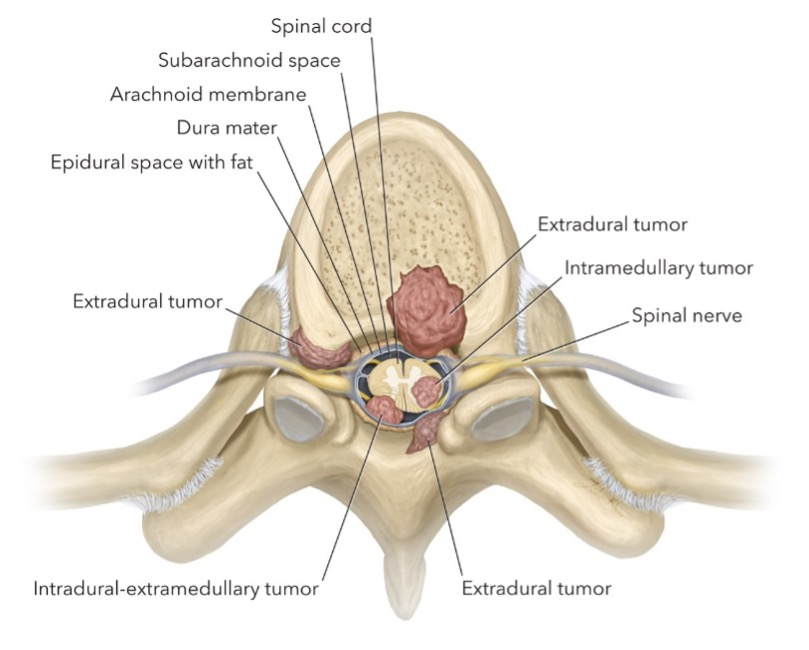
Illustration showing a spinal tumor and potential nerve/spinal cord compression.
Why Symptoms Happen
Tumors can cause pain by irritating surrounding tissues, weakening bone, or creating inflammation. If a tumor compresses a nerve root or the spinal cord, symptoms may include radiating pain, numbness, tingling, weakness, balance changes, or coordination issues.
When It Needs Prompt Evaluation
Progressive weakness, numbness, balance/coordination changes, or new bowel/bladder symptoms should be evaluated urgently, especially when symptoms are worsening or occurring with night pain or unexplained systemic symptoms.
Symptom Check
This quick check helps flag concerning symptom patterns that deserve faster evaluation. It’s not a diagnosis.
Spinal Tumor Triage
5 questions • flags urgency and next steps
1) Any urgent symptoms right now?
2) How long has the pain/symptoms been going on?
3) Is the pain worse at night or at rest?
4) Any systemic symptoms?
5) Are there nerve symptoms?
Diagnosis
Diagnosis begins with a thorough clinical evaluation and neurological exam. Imaging helps identify the tumor’s location, size, and involvement of bone or neural structures. In many cases, additional testing is required to confirm tumor type.
Clinical Exam
- Detailed symptom review and medical history
- Strength, sensation, reflex, and gait evaluation
- Assessment for spinal stability and pain pattern
Imaging
- MRI (best for spinal cord, nerves, and soft tissue)
- CT (bone involvement and structural detail)
- X-rays (alignment, fractures, stability)
Additional Testing
- Lab testing (selected cases)
- Biopsy (to confirm tumor type when indicated)
- Oncology coordination if cancer is suspected
Treatment
Treatment depends on the tumor type, location, size, and whether the spinal cord, nerves, or spinal stability are affected. The plan may involve a spine specialist, oncology team, radiation oncology, and other experts.
Non-Surgical / Medical Options
- Observation with close monitoring (selected benign tumors)
- Pain management and anti-inflammatory medications (when appropriate)
- Bracing for stability (selected cases)
- Radiation therapy (when indicated)
- Chemotherapy or targeted therapy (when indicated)
Surgical Options
- Tumor resection (removal) when appropriate
- Decompression to relieve pressure on spinal cord/nerves
- Spinal stabilization/fusion if the spine is weakened
- Minimally invasive approaches when appropriate
Recovery
Recovery depends on tumor type, location, and treatment approach. Some patients need rehabilitation to restore strength and mobility, while others focus on symptom control and ongoing tumor treatment.
After Diagnosis
- Care plan tailored to tumor type and severity
- Coordination with oncology when needed
- Monitoring for neurological changes
After Surgery
- Early mobility is encouraged in most cases
- Restrictions depend on procedure and stability needs
- PT may be recommended for recovery
Ongoing Treatment
- Follow-up imaging and surveillance
- Rehab for function and fall-risk reduction
- Symptom management as treatment continues
Prevention
Many spinal tumors cannot be prevented. The best approach is early evaluation for persistent or unexplained symptoms—especially when pain is worsening, occurring at night, or paired with neurological changes.
When To Seek Evaluation
- Persistent pain that doesn’t improve over time
- Night pain or pain at rest
- New or worsening nerve symptoms
- Unexplained systemic symptoms (selected cases)
Spine Health Habits
- Maintain strength and mobility as tolerated
- Use safe lifting mechanics
- Stay active with low-impact conditioning
- Follow treatment plans and surveillance when recommended
FAQ
Are spinal tumors always cancer?
No. Some spinal tumors are benign (non-cancerous). Others are malignant, and some are metastatic tumors that spread from another cancer. Imaging and sometimes biopsy help determine tumor type.
What symptoms are most concerning?
Progressive weakness, worsening numbness, balance issues, night pain, or new bowel/bladder changes are concerning and should be evaluated promptly.
How are spinal tumors treated?
Treatment depends on tumor type and location and may include observation, medications, radiation, chemotherapy/targeted therapy, and/or surgery to remove the tumor, decompress nerves, or stabilize the spine.
Schedule a consultation
We’ll review symptoms and imaging and coordinate next steps with the right team.
If you have progressive weakness, falls, or bowel/bladder changes, seek urgent evaluation.
What to bring
- Prior MRI/CT/X-ray reports (if available)
- List of current medications
- Any cancer treatment history (if applicable)
- Timeline of symptoms and progression
