Thoracic Stenosis
Thoracic stenosis occurs when the spinal canal narrows in the mid-back (thoracic spine) and compresses the spinal cord or nearby nerves. Symptoms can include mid-back pain, numbness, weakness, balance changes, and leg heaviness.
Common Symptoms
- Mid-back pain or stiffness
- Numbness or tingling in the trunk or legs
- Leg weakness, heaviness, or fatigue
- Balance changes or difficulty walking
- Band-like tightness around the chest/abdomen (some patients)
Common Causes
- Degenerative arthritis and bone spurs
- Thickened ligaments (ligamentum flavum)
- Disc bulging or herniation in the thoracic spine
- Less commonly: fractures, tumors, or congenital narrowing
Insurance check, handled.
We’ll verify benefits and walk you through expected coverage before treatment.
- Benefit verification before major steps
- Clear next steps + documentation help
- Scheduling support from our team
What Is Thoracic Stenosis?
Thoracic stenosis is narrowing of the spinal canal in the thoracic spine (mid-back). The thoracic canal contains the spinal cord, and when the canal becomes too tight, it can compress the cord and affect sensation, strength, and walking ability.
Thoracic stenosis is less common than cervical or lumbar stenosis. Because the spinal cord runs through the thoracic region, compression can produce symptoms in the legs, balance, and coordination, sometimes with a band-like sensation around the chest or abdomen.
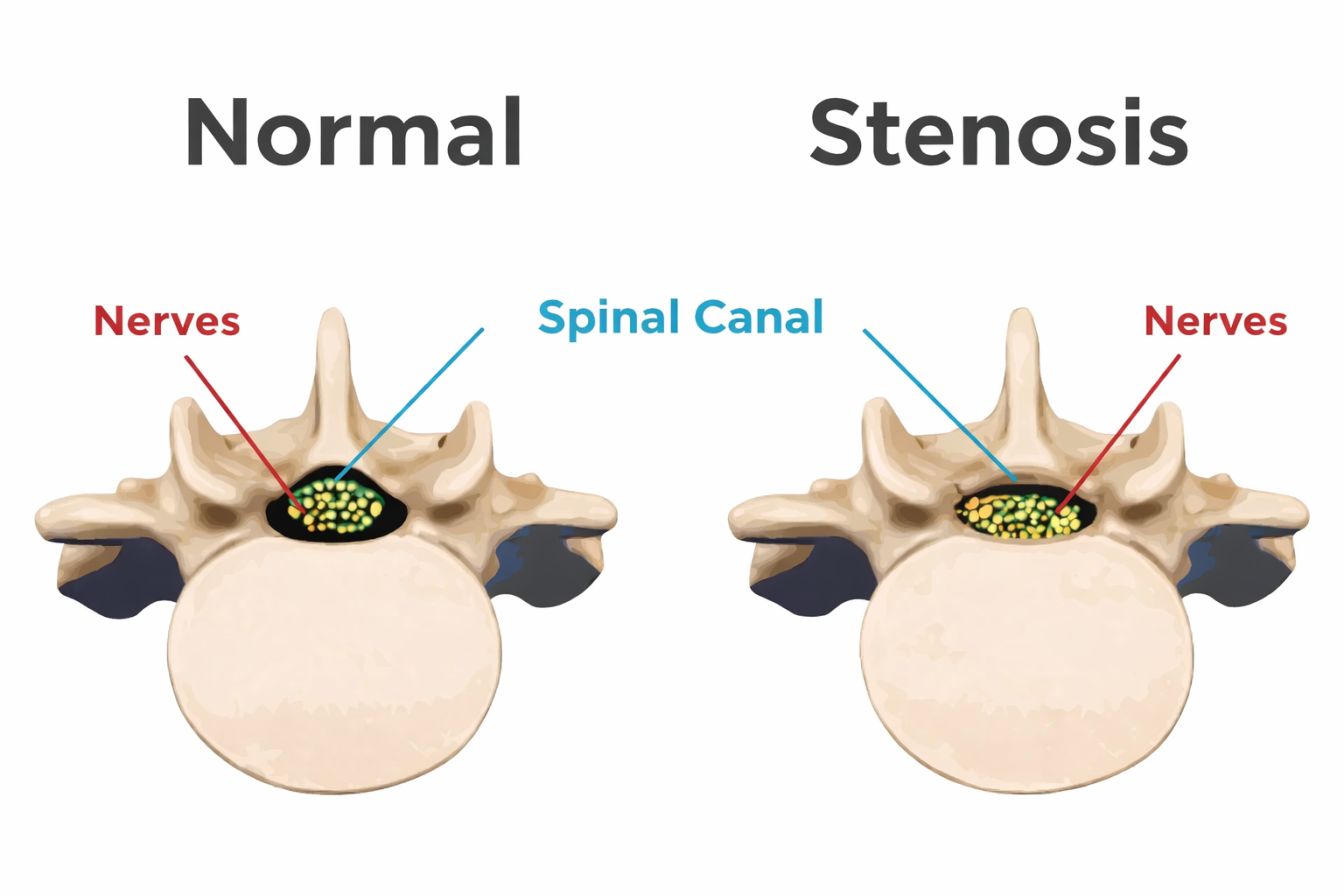
Illustration showing spinal canal narrowing (stenosis) that can compress the spinal cord.
Why It Happens
Thoracic stenosis may develop from degenerative changes such as arthritis, bone spurs, ligament thickening, and disc degeneration. In some cases, trauma, fractures, or other structural issues can contribute to narrowing.
When It Needs Prompt Evaluation
Progressive leg weakness, worsening balance, frequent falls, or new bowel/bladder changes can be signs of spinal cord compression and should be evaluated promptly.
Symptom Check
This guided check helps sort common symptom patterns seen with thoracic spinal cord compression. It’s not a diagnosis—if symptoms are concerning, schedule an evaluation.
Thoracic Stenosis Triage
5 questions • takes about 30 seconds
1) Any red-flag symptoms?
2) Leg heaviness or fatigue when walking?
3) Any balance/coordination changes?
4) Any numbness/tingling pattern?
5) Are symptoms progressing?
Diagnosis
Diagnosis starts with a focused neurological exam and symptom review. Imaging confirms the level and severity of thoracic canal narrowing and helps determine whether the spinal cord or nerve roots are being compressed.
Clinical Exam
- Strength, sensation, and reflex testing
- Gait, balance, and coordination evaluation
- Assessment of leg heaviness and endurance
Imaging
- MRI (best for spinal cord and soft tissue)
- X-rays (alignment and degeneration)
- CT or CT myelogram (selected cases)
Additional Tests
- EMG/NCS (if needed for nerve evaluation)
- Specialist review of imaging and symptoms
- Additional workup in selected cases based on findings
Treatment
Treatment depends on symptom severity and whether the spinal cord is being compressed. Mild symptoms may start with conservative care, while progressive neurological deficits may require surgical decompression.
Non-Surgical Options
- Activity modification and symptom management
- Physical therapy focused on mobility and safe strengthening
- Anti-inflammatory medications (NSAIDs) when appropriate
- Short-term oral steroids (selected cases)
- Posture and ergonomics to reduce strain
- Close monitoring for progression
Surgical Options
- Thoracic decompression procedures (when indicated)
- Laminectomy to relieve spinal cord pressure
- Decompression with stabilization if needed
- Treatment tailored to the specific cause (disc, bone spur, ligament)
Recovery
Recovery depends on the cause of stenosis, the degree of spinal cord involvement, and the treatment plan. Some patients improve with conservative care, while others may require surgery to stop progression.
Conservative Care
- Best for mild, stable symptoms
- Focus on mobility, strength, and symptom control
- Regular follow-up is important
After Surgery
- Early mobility is encouraged in most cases
- Restrictions depend on the procedure performed
- Physical therapy may be recommended
Expected Progress
- Improvements may continue over months
- Earlier treatment often leads to better outcomes
- Main goal may be preventing worsening
Prevention
Not all causes are preventable, but maintaining healthy spine habits can reduce flare-ups and support long-term back health.
Daily Habits
- Maintain good posture and core support
- Take breaks from prolonged sitting
- Use proper lifting mechanics
- Stay active and manage weight when appropriate
Strength & Mobility
- Core and upper back strengthening
- Thoracic mobility and flexibility work
- Low-impact conditioning consistency
- Balance training when appropriate
Related Conditions
Thoracic stenosis can overlap with disc degeneration, arthritis, and spinal cord compression. These pages cover common related diagnoses.
FAQ
Is thoracic stenosis common?
Thoracic stenosis is less common than cervical or lumbar stenosis. Because the spinal cord runs through the thoracic spine, symptoms may involve balance, coordination, and leg function.
Can thoracic stenosis cause leg weakness?
Yes. Compression of the spinal cord in the thoracic spine can cause leg weakness, heaviness, numbness, and walking difficulty.
When is surgery considered for thoracic stenosis?
Surgery may be considered when symptoms progress, neurological deficits develop, or imaging confirms significant spinal cord compression. The goal is to decompress the spinal cord and prevent worsening.
What test is most useful to confirm thoracic stenosis?
MRI is usually the most helpful because it shows the spinal cord, discs, and soft-tissue causes of narrowing. CT or CT myelogram may be used in select cases.
Schedule a consultation
We’ll review symptoms, imaging, and next steps. If you’re noticing worsening walking/balance or weakness, mention that when scheduling.
If you have severe or rapidly worsening symptoms, seek urgent evaluation.
What to bring
- Prior MRI/CT reports (if available)
- Medication list
- Timeline of symptoms (what’s changing?)
- Any fall history or gait/balance notes
